Are we any closer to a cure for cancer?
 May 2, 2023 | Dubai, UAE
May 2, 2023 | Dubai, UAE 
^BCervical cancer cells.^b Coloured scanning electron micrograph (SEM) of two cervical cancer cells after having undergone division from one cell. They are still joined by a narrow cytoplasmic bridge (at centre). These large rounded cells have an uneven surface with many cytoplasmic projections which may enable them to be motile. Typically, cancer cells are large and they divide rapidly in a chaotic manner. Clumps of these cells form tumours which possess the ability to invade and destroy surrounding tissues. Cancer of the cervix (the mouth of the womb) is one of the most common cancers affecting women. It can be fatal. Magnification unknown.
It was at the height of the COVID-19 pandemic, when the attention of the global media was understandably elsewhere, that news emerged of an unexpected silver lining – a clue in the hunt for a ‘vaccine’ for cancer.
The inoculations that finally freed society from the pandemic were based on messenger RNA (mRNA) technology. It transpires that the same mRNA technology that instructs cells to create proteins for counteracting COVID-19 could also trigger the production of cancer antigens for priming the immune system against tumors.
Scientists had long been eyeing mRNA as a revolutionary weapon in the war against cancer. The avalanche of funding, resources and talent that poured into the mRNA field heralded a game-changing moment in cancer research. It promised nothing less than a new breed of mRNA treatments designed to boost the body’s immune response against unwanted cell mutation.[1]
Now, scores of clinical trials are under way on patients with different strains of the disease, including melanoma, pancreatic and colorectal cancers. As data from these trials emerges in the coming years, we will learn just how significant this new technology is neutralizing humanity’s oldest and most deadly foe.
Even if mRNA exceeds expectations, it is unlikely to be effective against all cancers or cure all patients. Cancer remains a towering threat, written into our genes and etched into our destinies. The numbers speak for themselves.
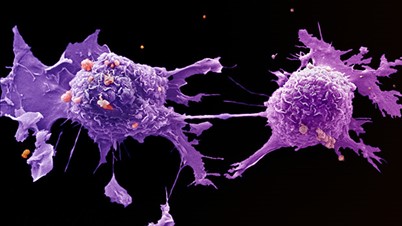
Image Credit: © LRI EM Unit
Cancer accounted for almost one in six deaths worldwide in 2020, or nearly 10 million fatalities – the leading cause of death globally.[2] In 2020, the most common causes of cancer deaths were:
- lung cancer (1.8 million deaths)
- colon and rectum cancer (916,000 deaths)
- liver cancer (830,000 deaths)
- stomach cancer (769,000 deaths)
- breast cancer (685,000 deaths)
Cancer is particularly cruel in that some of its deadliest forms, above, are also among the most pervasive. Leading cancers by rate of new diagnoses in 2020 were:
- breast (2.26 million cases)
- lung (2.21 million cases)
- colon and rectum (1.93 million cases)
- prostate (1.41 million cases)
- skin (non-melanoma) (1.20 million cases)
- stomach (1.09 million cases)
Stomach cancer has a five-year survival rate of 20%.[3] Lung cancer’s five-year survival rate is just 15%.[4] Cancer is as lethal as it is commonplace. Its resistance to treatment stems from the fact that it is not one disease, but many.

Traditional treatments falling short
Cancer is, in fact, a group of more than 100 related yet distinct conditions. It begins in the body’s cells, trillions of which grow, replicate and die during your lifetime. Cancer is merely a word for when this process deteriorates and cells acquire DNA variants causing them to grow improperly.
Maybe your body keeps making new cells for no purpose, or abnormal ones fail to expire as they should – either way, normal functioning cells are swamped by these rogue elements, preventing a particular part of the body from performing properly.
Cancers are either hematologic blood cancers (leukemias, lymphomas or multiple myelomas) or solid tumor cancers in organs and tissue. They can be benign – unable to spread beyond point of emergence – or malignant – liable to metastasize (or spread) around the body.
Early detection is crucial for positive outcomes. If diagnosed early, the survival rate for patients with eight of the most common cancers is more than three times higher than for patients diagnosed later. If diagnosed at stage one or two, more than 80% of cancer patients are still alive after a decade, falling to 25% for those diagnosed at stages three or four.[5]
Traditional treatments have varied widely in their approach and, crucially, in their effectiveness.
The most radically interventional treatment is, of course, surgery – in other words, the tactical removal of any malfunctioning cells en masse from their core site. Other treatments are less invasive than the knife. Radiotherapy uses high energy x-rays to destroy cancer cells at source. Chemotherapy, on the other hand, deploys anti-cancer cytotoxic drugs to attack cells from within. Hormonal therapy blocks essential hormones from reaching cancer cells, causing them to perish . Stem cell or bone marrow transplants, meanwhile, allow the body to withstand higher-dose treatments by bolstering the immune system.

These strategies, while often partially effective, are not free of problems or risk.
Of course, surgery only works on solid mass tumors rather than blood-borne cancers dispersed throughout the body. Even with solid mass tumors though, surgery might not always be an option; if the growth is located in a delicate place, such as the spinal column or brain, the risk of damage to surrounding tissue is too great. And even if an operation is viable, it is not always possible for a surgeon to remove all affected tissue because cancer exists at a microscopic cellular level. Any cancerous tissue left behind can start breeding abnormal cells once more.
Radiotherapy inevitably affects healthy cells as well as cancerous cells, leading to a range of complications including fatigue, difficulty swallowing food and shortness of breath. Radiotherapy also relies on every tumor site being known, whereas in reality many abnormal cell clusters are invisible to x-rays.
Chemotherapy generally declines in effectiveness as the body (and likewise the cancer) adapts to its presence – the challenge known as ‘drug resistance’. Naturally-occurring molecular changes within even a small number of cells can leave them immune to treatment. These resistant cancer cells can then grow and form new tumors causing patient to relapse within years, months or even weeks of treatment commencing.
None of these drawbacks and limitations even begin to acknowledge the central injustice of cancer treatment: the geographical lottery.
According to World Health Organization statistics, there are huge variations in the delivery of cancer treatment worldwide. Comprehensive treatment is offered in more than 90% of high-income countries, but in only 15% of low or middle income countries (LMICs).[6]
Such disparities are, quite literally, a matter of life and death.
Despite the incidence of cancer being lower in LMICs than in the developed world, mortality rates are notably higher.
Two-thirds of people with cancer in LMICs will die from their disease, compared with less than 50% in developed nations.[7]
This troubling trend is set to continue. A decade ago, some 65% of global cancer deaths occurred in LMICs. A decade from now, that figure is expected to hit 75%.[8] This is due not only to a rise in trigger factors within LMICs (poor diets and an increased use of alcohol and tobacco) but also rising rates of infection-associated cancers such as gastric, hepatocellular and cervical cancers.
Globally, while approximately 60% of new cancer cases emerge in LMICs, these countries attract less than 5% of cancer funding.[9] Oncology costs typically rise 7% to 10% annually, placing an unsustainable burden on those societies that can least afford it.

In the developed world we have an obligation to research and fund new cancer treatments, and to democratize access to them. But there is hope, with a raft of new cancer treatment strategies showing potential to transform outcomes for patients across the globe.
New strategies promise better outcomes
One of the most promising developments lies in the field of ‘precision oncology’. Just as no two people are exactly alike, nor are any two cancers. Precision oncology works by focusing on the specific molecular characteristics and genetic profiles of tumors within individuals. Such ‘single-cell’ profiling can help characterize cancer cells with unprecedented accuracy, allowing medics to manipulate genes via groundbreaking CRISPR genome editing.
CRISPR stands for Clustered Regularly Interspaced Short Palindromic Repeats, though its performance is more impressive than its acronym. If you are receiving CRISPR treatment then doctors will remove from your body a sample of T-cells (white blood cells in the immune system) ready for bespoke editing. They will delete several genes from these cells using a precise cutting tool and insert in their place receptors designed to bond with your own unique tumor cells. Millions of these augmented T-cells will then be grown in the lab ready for infusion back into your body, newly-equipped with the ability to assimilate and kill cancerous cells.

Using precision oncology techniques such as these, doctors can identify changes in cells that might promote tumor growth – and they can attack these hotspots while sparing healthy neighboring cells. In time, such Next Generation Sequencing (NGS) methods will grant patients access to personalized treatment regimens with better outcomes for both survival and quality of life.
Beyond CRISPR and precision oncology, other exciting developments are gradually shifting the odds in our fight against cancer.
When devising a cancer treatment plan, knowledge and speed are of the essence. Conventional biopsies are invasive, infection-prone and take time to scrutinize. Fortunately, rapid progress is under way in the field of liquid biopsies, where blood samples are screened for telltale signs of cancer. Nascent ‘synthetic biopsies’, meanwhile, promise to trick cancerous cells into producing biomarkers which can be more readily detected during screening.
The digital realm likewise promises to have a transformative effect on cancer treatment and care. AI-based risk analysis tools will help to prioritize preemptive screenings, leading to earlier than ever cancer detection rates. This is a vital step forward because, depending on the type of cancer involved, survival rates are up to 13 times higher if detected at Stage 1 than at Stage 4.[10] Faster internet connectivity globally will allow for the remote processing of biopsies. Together with digital health records, cloud-based data capture and apps, and a new generation of powerful technologies such as iSono Health’s FDA-approved ATUSA system (see below), AI will help unite patients with the care packages they need.
In the laboratory, the experimental drug guadecitabine, a DNA hypomethylating agent, is showing particular promise. Combined with traditional treatments, guadecitabine prevents patients becoming resistant to immunotherapy. In trials it halted the spread of cancer in a third of patients.[11]
Another strategy gaining momentum involves the ‘microbiome’ – the mass of microorganisms living within our bodies. Manipulating the microbiome, it turns out, can help boost suppressed immune systems in cancer patients. And that’s not all. The microbiome also contains peptides that can mimic antigens on the surface of tumors, unmasking any tumors previously invisible to the immune system and rendering them vulnerable to attack. Microbiome-based cancer vaccines are currently awaiting human trials.
Ultimately, prevention is better than cure, and that is why DNA samples from thousands of cancerous tumors are being studied in the UK to reveal their mutational triggers: internal cell malfunctions, carcinogens from smoking, or exposure to UV light.[12] Analyzing genetic data in this way could help decrease the future incidence of cancers globally.
Paying for these state-of-the-art oncological treatments, however, will require similarly innovative solutions.
Private sector can help meet cancer’s colossal cost
Combating cancer is a costly business. Stomach and lung cancer drugs can cost up to US$ 12,000 a month, with some leukemia treatments topping US$ 64,000. More effective cancer screening devices and refined genome sequencing technologies are vital to unlocking affordable treatments. Yet with new drug development costing upwards of US$ 1 billion per product, governments alone cannot meet the endless financial burden of research and development.[13]
We in the private sector have both the obligation and the opportunity to make a transformational impact on cancer care worldwide. We can help patients live longer, more comfortable lives.
At Abdul Latif Jameel Health, we are channeling the power of our private capital into a range of startups promising oncology care breakthroughs.
We have joined forces with San Francisco-based iSono Health to bring the world’s first AI-driven portable 3D breast ultrasound scanner to the global south – potentially helping millions of women in the developing world access meaningful cancer treatment.
iSono Health’s FDA-approved ATUSA system allows for automated whole-breast ultrasound imaging at point of care, without need for trained operators. The device connects to a laptop or tablet for real-time 3D image visualization, integrating seamlessly with machine learning models to offer physicians a comprehensive set of tools for better decision making. The agreement with iSono Health will see Abdul Latif Jameel Health distribute these scanners across the Middle East, Africa and Asia.
We are also helping to fund Massachusetts-based EQRx, a pharmaceutical company committed to developing and delivering vital new drugs at significantly lower prices across the developing world. Its drugs Aumolertinib (an epidermal growth factor receptor inhibitor) and Sugemalimab (an anti-PD-L1 antibody) have shown positive data from Phase III studies in the treatment of non-small cell lung cancers. EQRx could eventually make cancer treatment more accessible and more affordable to millions of people in emerging markets.
In addition, we are working with biotech company Evelo Biosciences. Evelo develops single-strain microbe medicines designed to act on the small intestinal axis. Among Evelo’s range of drugs in development is EDP1908, designed for tumor suppression in cancer patients.
Meanwhile, the Butterfly iQ+ device developed by another Abdul Latif Jameel Health partner, pioneering healthtech firm Butterfly Network, is the world’s only single-probe, whole-body, imaging machine. It could enable medical imaging to be carried out in remote communities for the first time – and has already demonstrated its ability to successfully diagnose cancer.
“With lifespans lengthening globally, it is believed that within a decade there will be 24 million new cancer sufferers in the world, many within deprived communities”, says Dr Akram Bouchenaki Chief Executive Officer of Abdul Latif Jameel Health. “That is 24 million lives in the balance, and 24 million families facing heartbreak and trauma.”

“By investing in new innovations in science and technology, we in the private sector can help maintain the pipeline of revolutionary drugs seeking to turn the tables on cancer.
In so doing we can offer fresh hope to patients worldwide, regardless of their place of birth, income level or social status.”
[1] https://www.cancer.gov/news-events/cancer-currents-blog/2022/mrna-vaccines-to-treat-cancer
[2] https://www.who.int/news-room/fact-sheets/detail/cancer
[3] https://www.cancerresearchuk.org/about-cancer/stomach-cancer/survival
[4] https://www.cancerresearchuk.org/about-cancer/lung-cancer/survival
[5] https://www.theguardian.com/society/2015/aug/10/cancer-survival-rates-higher-early-diagnosis
[6] https://www.who.int/news-room/fact-sheets/detail/cancer
[7] https://www.weforum.org/agenda/2022/02/cancer-care-future-technology-experts/
[8] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6452918/
[9] https://www.sciencedirect.com/science/article/pii/S2059702920323358
[10] https://www.weforum.org/agenda/2022/02/cancer-care-future-technology-experts/
[11] https://www.theguardian.com/science/2022/aug/22/new-cancer-treatment-offers-hope-to-patients-immunotherapy-resistant
[12] https://www.cam.ac.uk/research/news/largest-study-of-whole-genome-sequencing-data-reveals-new-clues-to-causes-of-cancer
[13] https://www.thenationalnews.com/health/2023/01/31/arab-health-overpriced-cancer-drugs-leave-billions-without-hope/
Related Articles
For press inquiries click here, or call +971 4 448 0906 (GMT +4 hours UAE). For public inquiries click here.